Onpoint Supports CMS's CPC+ Data Feedback Reporting with Generation of Performance Measures
May 2017 -- Onpoint and its partners, prime contractor Deloitte Consulting, LLP, and Econometrica, Inc., were selected last fall by the U.S. Centers for Medicare and Medicaid Services (CMS) to develop actionable reporting at both the regional and primary care practice settings in support of the Comprehensive Primary Care Plus (CPC+) national medical home initiative. The CPC+ program aims to strengthen primary care through regionally based multi-payer payment reform and care delivery transformation.
These "feedback" reports developed by Deloitte are distributed to more than 2,800 participating CPC+ primary care practices across 14 CMS-selected regions nationally – from Rhode Island to Oregon to Hawaii – comprising more than 13,000 physicians and serving more than 1.76 million Medicare beneficiaries. Onpoint’s role in the project is to lead the design, development, and generation of the Deloitte-defined set of cost, quality, and utilization measures that are incorporated into the suite of reporting.
For each feedback report, data is broken down into four key subject areas that feature reporting across multiple measures, including expenditures and utilization metrics:
- Performance Highlights: Information includes five rolling-quarter trends and rates of change for total beneficiaries attributed to a practice, total number of practitioners per practice, expenditures per beneficiary per month (PBPM), observed versus expected hospitalizations, and observed versus expected emergency department visits.
- Demographics: Data in the demographics section examine the breakdown among the attributed beneficiaries for that practice over CPC+ risk tiers, age, race/ethnicity, and gender categories.
- Expenditures: PBPM information is provided for inpatient, acute inpatient, outpatient, professional, post-acute, and specialty costs. Also included is a breakdown of where the primary care dollars for beneficiaries attributed to a particular practice are being spent – examining the question of whether beneficiaries are receiving primary care from their attributed practice or instead are seeking primary care services from other practices nearby. Similar to the demographics section, high-level information for the region also is supplied for comparative purposes.
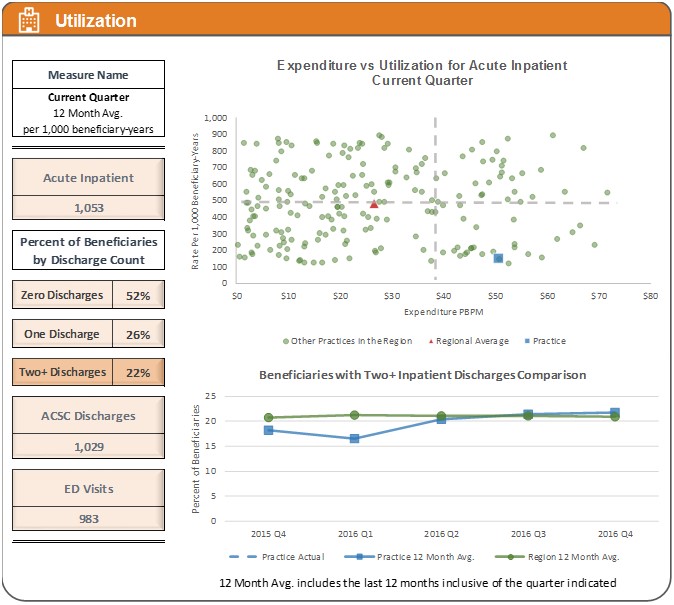
- Utilization: The utilization data provide a practice-to-region scatterplot of expenditure versus utilization data for acute inpatient claims data. Also provided are discharge rates for beneficiaries with ambulatory care sensitive conditions, emergency department visits, and a practice-to-region comparison of attributed beneficiaries that have had one, two, or more discharges over the preceding 12-month period.
The feedback reports disseminated to the participating CPC+ practices have been well received so far. As Onpoint and our partners look ahead to the next round of reporting, additional measures and metrics, including a breakout of specialty expenditures, a closer look at chronic conditions, and more, are in the queue for development. Follow-on reporting for the CPC+ practices will be released on a quarterly schedule, with the next round to be distributed in July 2017.