Using HealthPartners’ TCOC Measurement System to Drive Insightful Analysis

Health transformation initiatives across the country are working hard to reverse many of the key drivers of healthcare spending by identifying areas of overuse and inefficiency. One key step in this effort is calculating a patient’s total cost of care and resource use, illuminating possible waste as well as potential cost-saving opportunities. While some total cost of care measures simply sum a patient’s payments and stop there, others use a much more advanced formula to dig deeper for more insightful analysis. Leading this latter breed is HealthPartners’ Total Cost of Care (TCOC) and Resource Use framework — a full-population, person-centered measurement tool designed to address and support researchers’ efforts to understand and slow the growth of healthcare spending.
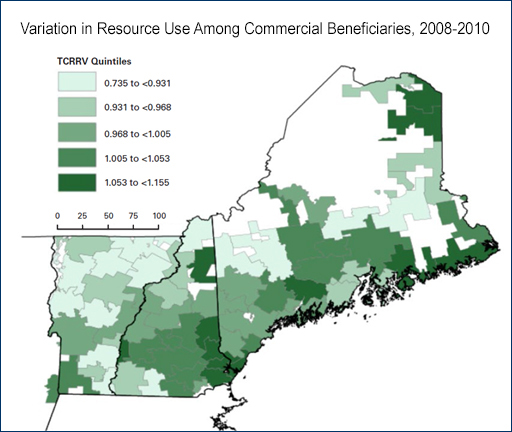
Onpoint has calculated HealthPartners’ TCOC and Resource Use measures for multiple projects, providing comparative reporting across states, providers, and practices. Our expanding work with the HealthPartners’ software kicked off several years ago when our team undertook the first multi-state integration of all-payer claims databases, bringing together commercial, Medicaid, and Medicare data for Maine, New Hampshire, and Vermont. This expansive data source served as the basis for our Tri-State Variation in Health Services Utilization & Expenditures in Northern New England study.
Following the report’s release, the Dartmouth Institute selected us as their data and analytic partner for two nationally recognized studies: The Dartmouth Atlas of Children’s Health Care in Northern New England and a multi-state analysis of HealthPartners’ TCOC measures through a distributed data model. In each case, Onpoint was responsible for the mapping and data normalization work required to support measures generation across multiple states with different collection rules and data standards and for generating the measures themselves — HEDIS-based quality measures for the Dartmouth Atlas and all measures for the TCOC demonstration and all.
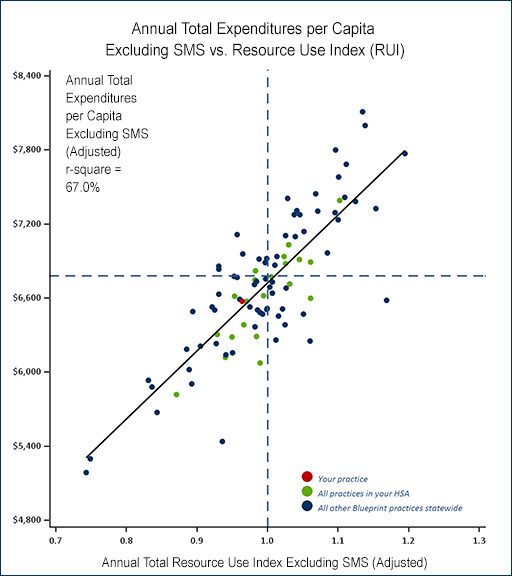
Onpoint has also applied the HealthPartners’ TCOC software to Vermont’s statewide commercial, Medicaid, and Medicare data in support of the Blueprint for Health advanced primary care program. We regularly produce scatter grams, for example, that demonstrate the positive correlation between risk-adjusted expenditures and risk-adjusted frequencies and intensities of services utilized for Blueprint’s participating practices. These graphics, which illustrate where practices fall along the high/low cost and utilization ranges, enabling comparative analyses at multiple levels, are being used by Vermont leaders in their efforts to develop an area-based payment model.
Explore More
- Indiana Health Prices Chatbot Recognized Nationally with NAHDO 2026 Innovation in Data Dissemination Award
- Staff Spotlight: Kate Davis, MBA, PMP - Client Services Manager
- New Onpoint Issue Brief: Calculating FFS Equivalents for Capitated Services
- Staff Spotlight: Jesse Drummond, PhD - Director of Data Analytics